Korea Sees Rising Glaucoma, Including Younger Adults, with Implications for U.S. Screening
Glaucoma remains one of the leading causes of irreversible blindness worldwide, alongside age-related macular degeneration and diabetic retinopathy. In Korea, experts say early symptoms are often subtle, making timely diagnosis and ongoing treatment essential to prevent permanent nerve damage. A Seoul-based ophthalmologist from Kangdong Kyunghee University Hospital notes that the condition is increasingly seen in younger adults, underscoring the need for vigilance even among the 20s and 30s.
Glaucoma is a progressive optic neuropathy driven by multiple factors, typically first narrowing peripheral vision before central vision is affected. Most patients do not notice symptoms in the early stages, and nerve damage can advance before a diagnosis is made. Acute angle-closure glaucoma is the notable exception, presenting with sudden eye pain, redness, headaches, nausea, and rapid vision loss, requiring emergency care.
Korean health data show a notable rise in glaucoma cases over a five-year span. According to the National Health Insurance Service’s statistics on diseases of public concern, the number of people treated for glaucoma rose from 967,554 in 2020 to 1,223,254 in 2024, a roughly 26 percent increase. While older adults in their 60s and above remain the largest group, the number of patients in their 20s and 30s also grew—from 104,348 to 118,106, an increase of about 13 percent—indicating a broader age distribution than before.
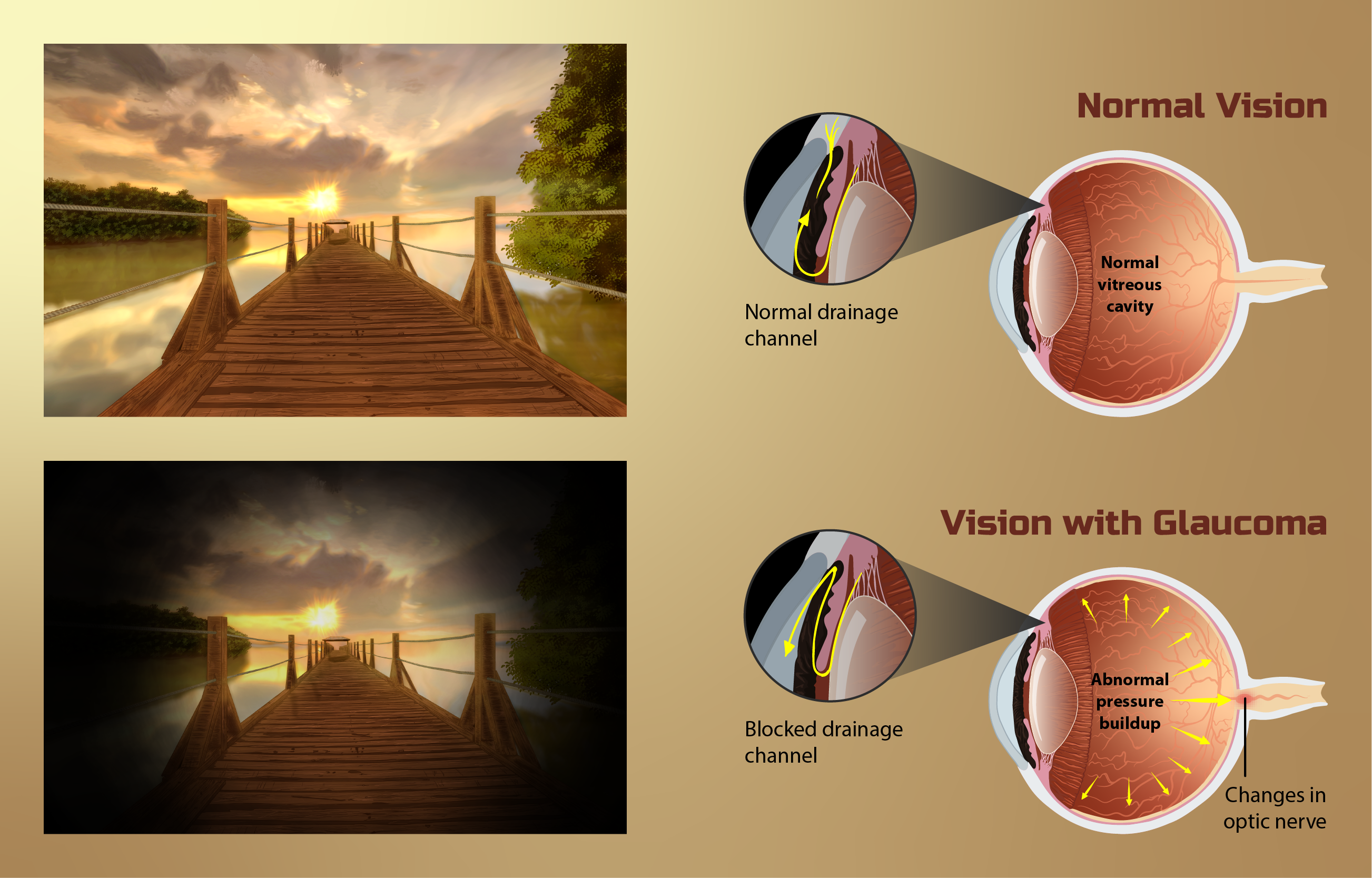
The most important risk factor is intraocular pressure, which, when elevated, damages the optic nerve and worsens vision loss if untreated. Importantly, some patients develop glaucoma despite normal-range eye pressure, known as normal-tension glaucoma. Other factors that can raise risk include a family history, high myopia (severe nearsightedness), thinner central corneal thickness, and compromised blood flow to the optic nerve. Even with normal IOP, these factors can justify regular screening, particularly for younger individuals with risk profiles.
Diagnosis combines several tests: measuring intraocular pressure, examining the optic nerve head with a fundus exam, and assessing the visual field. Optical coherence tomography and other imaging help quantify nerve damage, while corneal thickness measurements improve the accuracy of IOP assessments—an important consideration for people who have undergone refractive surgery. In some cases, additional tests may be used to distinguish glaucoma from other optic diseases.
Treatment begins with eye drops to lower intraocular pressure and lessen nerve strain. If medications fail to control the disease, laser or surgical options are considered. Laser therapies such as trabeculoplasty and surgical approaches like trabeculectomy or implantable drainage devices are common. In recent years, minimally invasive glaucoma surgery (MIGS) has gained traction as a safer, quicker option with faster recovery, though it may offer less dramatic IOP reduction compared with traditional surgery, so patient selection and long-term outcomes remain under study. Acute-angle glaucoma requires rapid IOP reduction followed by procedures such as laser iridotomy to restore drainage pathways.
For those at higher risk—typically adults over 40, individuals with high myopia, and people with a family history—annual comprehensive eye exams are recommended even in the absence of symptoms. Other risk enhancers include prolonged steroid use and conditions such as diabetes and high blood pressure. Park Sehee, a professor of ophthalmology at Kangdong Kyunghee University Hospital, emphasizes that early detection and treatment are the surest way to preserve vision over a lifetime, and that proactive screening remains essential even for younger patients with risk factors.
Beyond Korea, the rise in glaucoma and the evolution of its treatment have global implications for the United States and other health systems. As populations age and screenable imaging becomes more widespread, early detection can reduce long-term costs and preserve function. The spread of options from traditional surgeries to MIGS, and the ongoing need for access to affordable medications and devices, highlight shared policy and market considerations for eye care, pharmaceutical supply chains, and the adoption of diagnostic technologies across borders.