South Korea pioneers noninvasive nasal stem-cell therapy for traumatic brain injury
A team led by Professor Park Chan-heum of Hallym University Chuncheon Sacred Heart Hospital has developed a noninvasive nasal-delivery method to administer stem cell therapy for traumatic brain injury. The approach aims to bypass brain surgery while delivering therapeutic cells and factors directly to the brain.
Traumatic brain injury is caused by sudden impact that damages neurons, often leading to cognitive and motor deficits. Traditional stem cell treatments require invasive brain injections and have shown limited cell survival. The researchers turned to the nasal cavity’s mucosa as a conduit to the brain, seeking a safer, scalable alternative.
In their process, the team mass-cultured mesenchymal stem cells in a bioreactor and shaped them into neural rosettes. These neural rosettes were then encapsulated in a specialized hydrogel containing silk fibroin to protect the cells and improve their survival after administration via the nose. The formulation also facilitates the release of therapeutic factors from the neural rosettes into damaged brain tissue.
Animal experiments modeled traumatic brain injury and demonstrated the treatment’s potential. Treated animals began to show brain-function recovery around day three, and by one week, they recovered at more than twice the pace of untreated animals. In key memory and learning regions, recovery-related molecular markers approached normal levels, and damaged neurons showed signs of revival along with sustained new neural tissue.
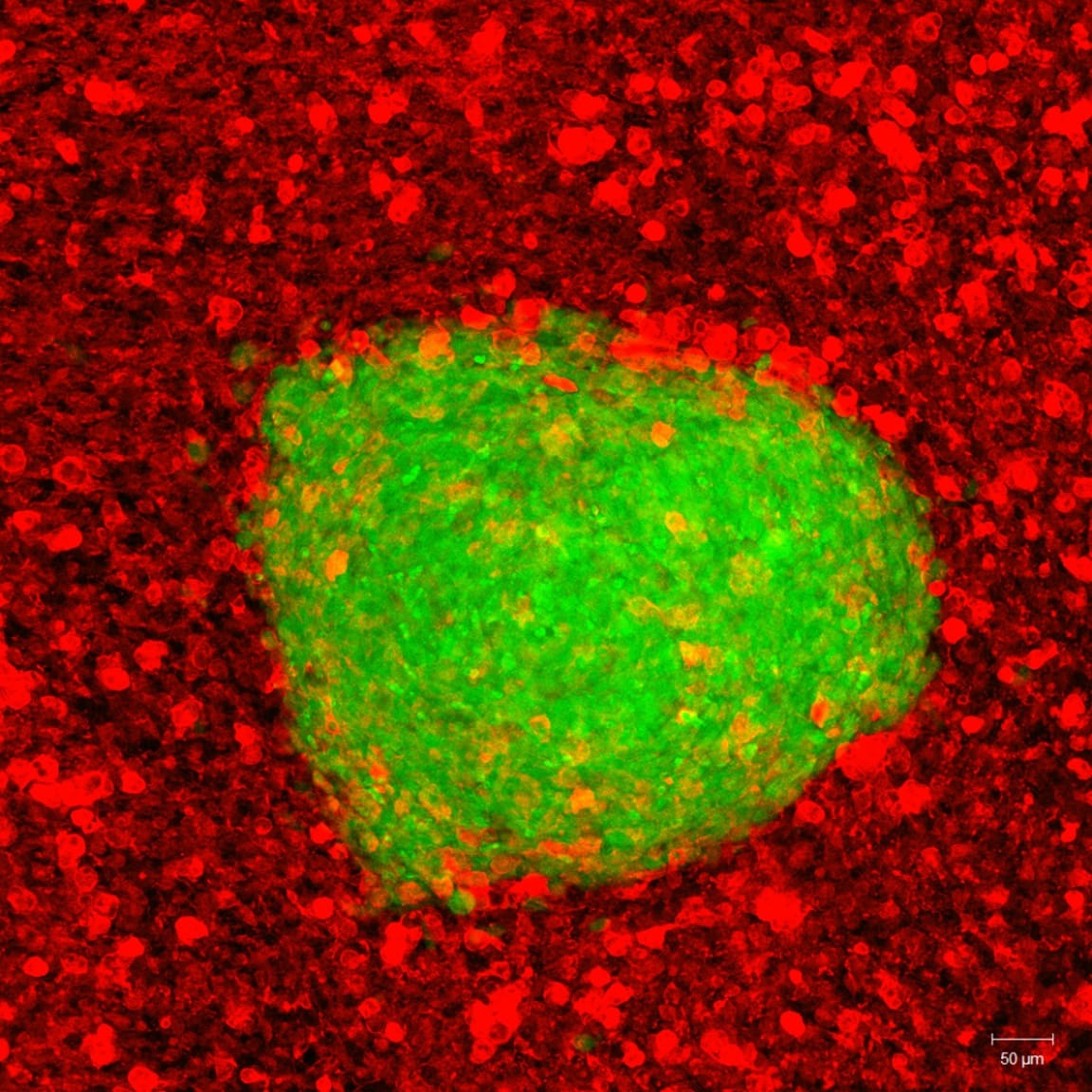
The study also reported a healthier brain environment post-treatment, with a marked reduction in toxic substances and stress factors associated with brain injury. Additionally, neural networks appeared more stable, suggesting protection against further network disruption after trauma.
Beyond efficacy, the researchers established a “master cell bank” using automated bioreactors to culture the mesenchymal stem cells that form the neural rosettes. Stored cells are maintained in small, organized aliquots, enabling rapid, consistent production of therapeutic cells while preserving their properties through storage and use.
The work, titled Hydrogel-based human umbilical cord-derived neural rosettes for noninvasive nasal delivery in acute neuroprotection after traumatic brain injury, was published in the January issue of APL Bioengineering. Park said the nasal, non-surgical delivery offers both safety and therapeutic benefit, and he suggested expanding this approach to other brain diseases such as Parkinson’s and Alzheimer’s.
For U.S. readers, the development highlights a potential paradigm shift in treating brain injuries and other neurodegenerative conditions. A noninvasive delivery platform paired with scalable manufacturing could influence future clinical trials, reduce surgical risks, and affect the broader biotech and pharmaceutical supply chains as cell therapies move toward commercial viability. The research also underscores the growing global interest in nasal-delivery strategies and standardized cell banks as means to accelerate treatment availability while maintaining quality and safety.