Korea expands national cancer screening to include colonoscopy by 2028
AI-driven health information, or “health intelligence” HQ, is emerging as a major trend in Korea. Yet greater access to information can backfire if people self-diagnose and skip necessary tests. A National Cancer Center survey on cancer screening behavior found that the single largest reason for not undergoing screening is the belief that one is healthy, cited by about 43.4% of respondents.
Among the six major cancers covered by Korea’s national screening program, colorectal cancer has the lowest participation, remaining in the 40% range. The six-screen program also includes stomach, liver, breast, cervical, and lung cancers, but colorectal screening lags behind despite rising risk.
Colorectal cancer often presents few early symptoms. When symptoms do occur, they may include blood in the stool, a feeling of incomplete evacuation, changes in stool caliber, dark stools, indigestion, fatigue, or abdominal pain. Symptoms can vary by tumor location: right-side cancers tend to cause anemia or a palpable mass, while left-side cancers more commonly cause constipation or bright red blood in stool.

Under Korea’s current national screening, adults 50 and older are offered an annual fecal immunochemical test (FIT) or fecal occult blood test. That test detects blood in stool but does not assess other signs of cancer, so regular colonoscopy is important for both early detection and prevention. The government is advancing a reform to include colonoscopy in the national screening program beginning in 2028.
Colonoscopy has a major advantage: it allows immediate treatment if polyps (adenomas) are found. More than 95% of colorectal cancers start from adenomas, and removing a polyp during colonoscopy can reduce cancer risk by up to 90%. When cancers are detected early, treatment can be limited to endoscopic procedures, with five-year survival for early-stage disease above 90%.
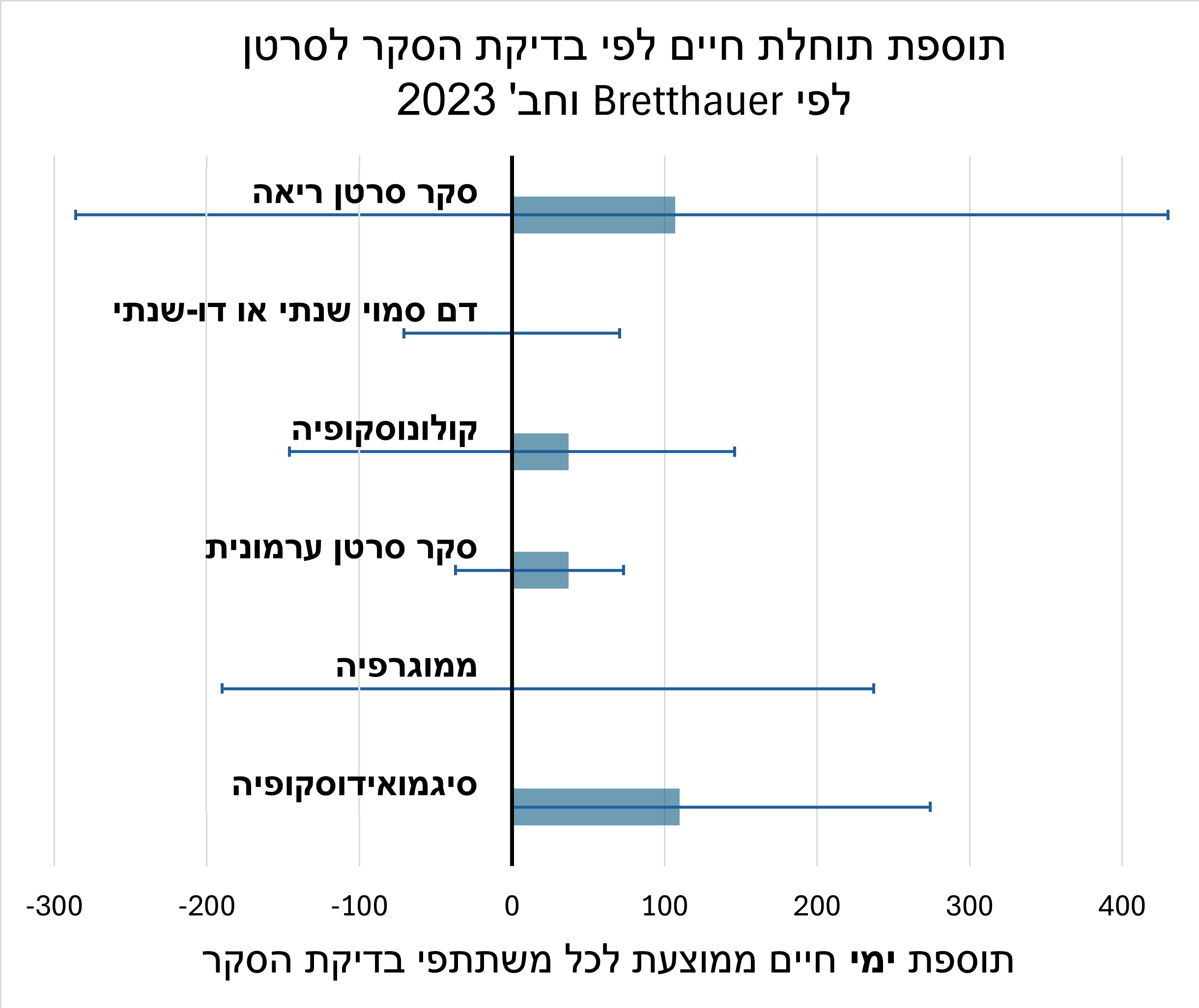
There is a growing trend toward screening at younger ages. In Korea, rising numbers of younger colorectal cancer patients have prompted recommendations for preventive colonoscopy starting at age 40 for those with risk factors such as family history, obesity, or smoking, even in the absence of symptoms.
Dr. Hong Jong-sam, head of the Health Medicine Center at Gangneung Asan Medical Center, stressed that polyp size matters: adenomas under 1 cm carry about a 1% future cancer risk, while those 2 cm or larger raise the risk to more than 40%. He urged relying on precise screening rather than online chatter as the first step in prevention.
The National Cancer Center’s planned expansion of colonoscopy in Korea’s screening program reflects a broader global emphasis on endoscopic screening as a preventive tool. For U.S. readers, the development underscores the importance of colonoscopy in reducing colorectal cancer mortality, potential implications for healthcare spending and device supply chains, and the ongoing policy discussions about how best to structure population-wide cancer screening and early intervention.